As Wuhan begins to restore “normal” operations and some countries across Europe and North America are seeing signs that some of the most acute risks of COVID-19 may be plateauing, the impacts of the virus and its toll upon populations and economies is just now reaching much of the developing world. And it is in these developing economies where the harmful – and potentially devastating – effects could be felt most acutely.
Less established and lower quality healthcare infrastructure in many developing economies will mean they are ill-equipped to manage the coming surge in acute care cases brought on by COVID-19. Lower baseline access to basic necessities such as food and sanitized water could amplify the effects of these dramatic shortages, causing service disruptions and limiting the ability to practice proper preventative measures. Compounding these risks, countries with less diverse economies may experience even more halting and destructive economic effects from industry shocks during this same time. In short, a perfect storm that we must all work together to mitigate.
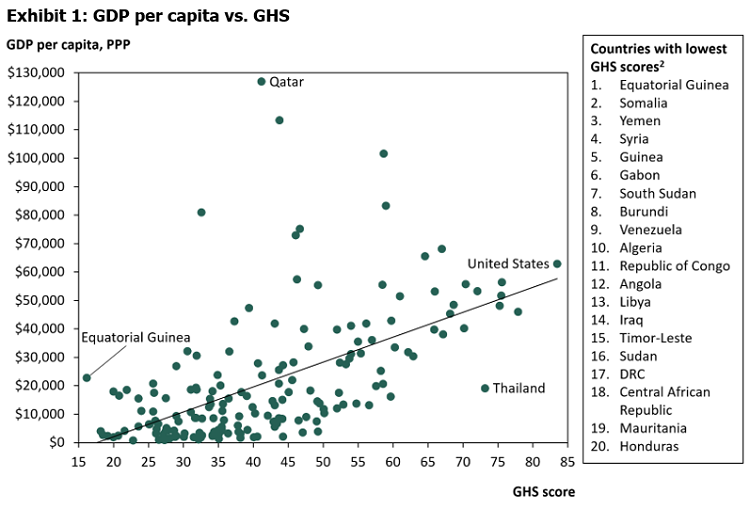
To properly understand the magnitude of these types of risks, a good starting point is the Global Health Security (GHS) Index, a measure of a country’s preparedness for a pandemic jointly created by the Nuclear Threat Initiatives (NTI), the Johns Hopkins Center for Health Security, and the Economist Intelligence Unit (EIU). The GHS index measures a country’s ability to prevent the emergence of pathogens, detect and report epidemics, rapidly respond to and mitigate the spread of epidemics, treat and protect the sick, comply with international norms, and manage overall risks.1 Y Analytics plotted the 195 countries ranked by the GHS to their GDP per capita on a purchasing-power-parity basis (Exhibit 1). Unsurprisingly, lower income countries tend to score lower on the GHS, indicating a poorer quality of healthcare infrastructure and less capability to manage the risks associated with COVID-19. However, as noted by the GHS, preparedness is not strictly determined by a country’s GDP per capita, as several middle- and low-income countries score higher on the index than other high-income countries. An example is Thailand, a middle income country whose health system ranks among top ten in the world, due to its strong healthcare capacity and ability to monitor and track infections.
We recognize that no two developing countries are the same, and that some may face more nuanced challenges during this time. Below we provide snapshots of vulnerabilities for specific populations.
Lack of economic diversity
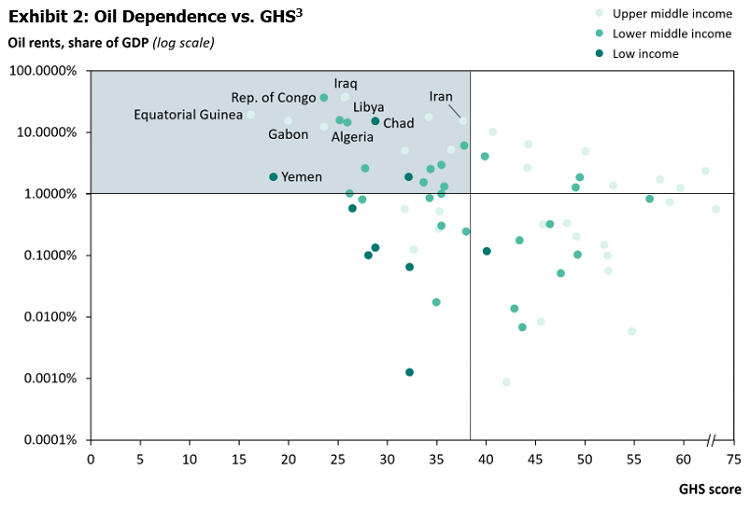
Economic dependence on sectors that are particularly depressed or volatile right now could exacerbate a country’s already limited ability to respond to the pandemic. For example, developing economies in the Middle East and Africa that have a high dependency on oil revenues may face the “dual shock” of stretched healthcare capacity and economic disruptions. Some of these countries, such as Iran, Iraq, and the Republic of Congo, where oil rents account for more than 10% of GDP, have confirmed tens of thousands of deaths associated with the pandemic (Exhibit 2). In addition to the challenge of managing mounting infections, these economies are also facing economic pressures as oil prices continue to face fluctuation in the near future. Some country leaders have called for greater international cooperation to manage the risks associated with these pressures.
Informal employment
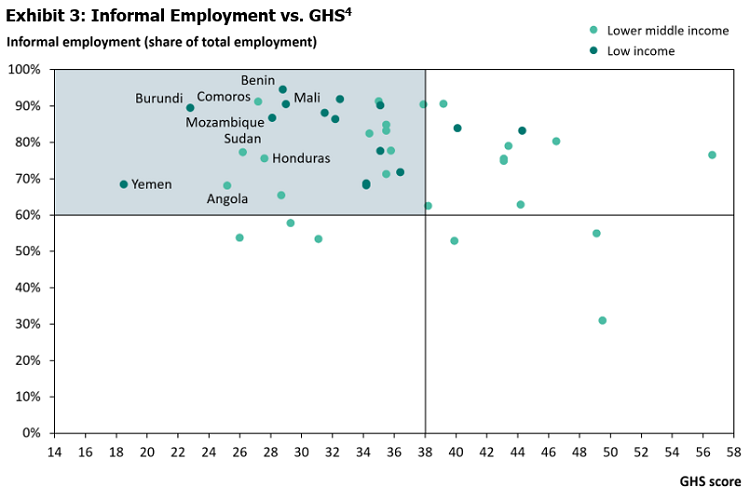
While experts agree that limiting physical social interaction is a crucial step towards managing the spread of infections, mandating shelter-in-place is challenging due to the disruptions it causes for workers and caregivers. These challenges are exacerbated in developing countries, where 93% of the world’s informal jobs are estimated to reside. The International Labour Organization (ILO) estimates that informality is highest in Africa at more than 85% of employment, followed by APAC, Arab States and Latin America & Caribbean, at 70%, 68%, and 53%, respectively (Exhibit 3).
For informal workers, reduced working hours means loss of income with no possibility of receiving unemployment benefits (ILO, Quartz Africa). Unsurprisingly, shelter-in-place and quarantine measures have inspired protests in cities with significant amounts of informality like Bogota and Kampala. To make lockdowns sustainable, different governments in developing countries have approved different economic packages to provide food, staples and subsidies, experimenting with different delivery channels ranging from neighborhood shops to government distribution centers and the conditional cash transfer networks. However, these programs are insufficient, and some of these individuals are harder to reach (WSJ).
Access to information
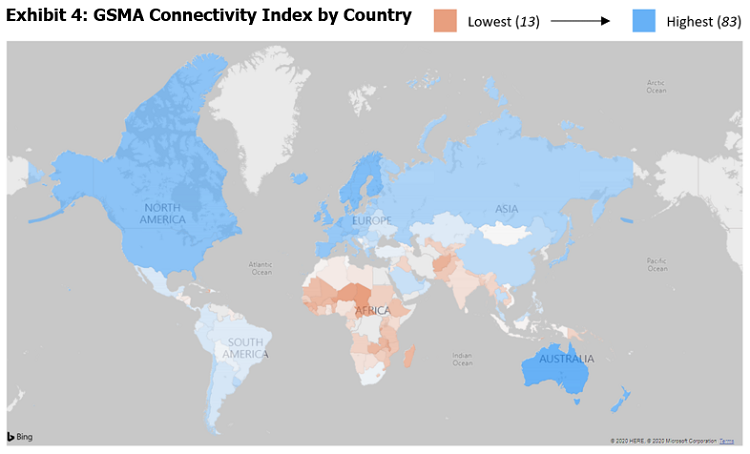
Another concern for developing countries is access to information. Under normal circumstances, a “digital divide” could put populations at risk of not being able to participate in the modern economy. The International Telecommunications Union found in 2019 that although 97% of the world’s population live in areas with some internet availability, only 53.6% are connected, signaling the gap between coverage and connectivity caused by tariffs, handset affordability, network performance, and more. The GSMA Mobile Connectivity Index measures the performance of 165 countries against key enablers of mobile internet adoption: infrastructure, affordability, consumer readiness, and content and services. Among the developing world, African and South Asian countries exhibit the lowest connectivity figures, while European, Latin American, and Caribbean developing economies have, in many cases, significantly invested in ICT over the past 10 years (Exhibit 4).
The current pandemic may make the concerns around existing digital divides more acute. Without reliable access to the internet, participation in remote lessons for the more than 1.4 billion learners worldwide whose schools have closed is difficult, if not impossible. Similarly, it may be more challenging for governments to track infections or disseminate information as has been done in South Korea and China (WEF 1, WEF 2).
Access to clean water
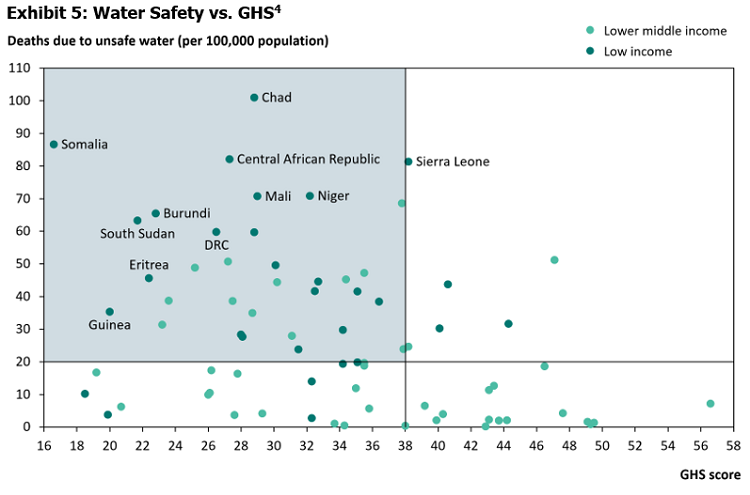
Despite the importance placed on proper hygiene during the global pandemic, many parts of the world still lack access to clean water. The WHO (2015) reports that only 30% and 47% of households in sub-Saharan Africa and South Asia, respectively, have access to improved sanitation facilities. Countries that lack access to clean water are already at risk of adverse health outcomes under normal circumstances. Ashbolt (2004) found that poor water quality and lack of sanitation and good hygiene account for some 1.7 million deaths a year worldwide. In countries like Chad and Somalia, more than 80 deaths per 100,000 people every year are caused by unsafe water (Exhibit 5). These countries’ ability to implement the preventative measures recommended by the WHO are significantly hampered by the lower baseline of access to water.
Refugee populations
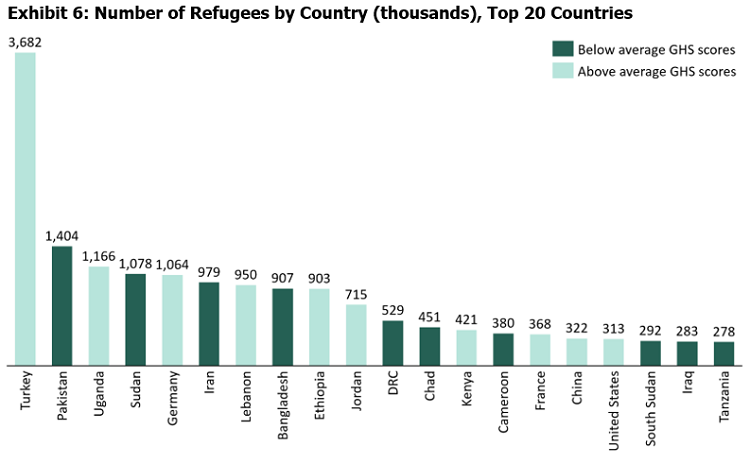
Among developing countries, refugees and migrants residing in camps are among the most vulnerable groups in the current context, given their living situation, inability to social distance, and diminished access to basic necessities. According to UNHCR, there are over 70 million people currently displaced around the world. Migrants and displaced individuals, like the 850,000 Rohingya refugees in Bangladesh, face particular danger due to a lack of resources and adequate physical infrastructure, as well as limited access to the host country’s national healthcare system. Indeed, a study of the 2009 H1N1 pandemic shows that the virus had spread quickly among refugees in the Myanmar region. Importantly, 10 out of the 20 countries with the highest refugee numbers have below-average GHS scores (Exhibit 6).
Depending on the characteristics of their health systems, basic infrastructure, and economies, developing countries, broadly, and those with vulnerabilities specific to the current crisis, in particular, could see larger disruptions as a result of COVID-19. To address these sensitivities, multilateral organizations like the World Bank, International Monetary Fund, Inter-American Development Bank, Asian Development Bank, and African Development Bank have pledged close to $300 Billion to support developing countries’ responses to the pandemic. Beyond multilateral organizations, leaders in the public and private spheres are investing in solutions to weather the current crisis. Countries like Portugal have offered citizenship rights to migrants and asylum-seekers to ensure they have access to healthcare. African mobile network operators are offering zero-rated access to essential websites and canceling fees for mobile money transfers to ensure uninterrupted access to critical information and web-related services. Companies in West Africa have banded together in the West Africa Private Sector Coronavirus Platform (WAPSCON19) with the hope of improving the livelihood and health of the wider community through information sharing and response coordination. These and more will be essential to the response in the most vulnerable developing countries.
Footnotes
- We note that there are other measures and indices that also aim to illustrate different countries’ preparedness for a pandemic. Another example is the Infectious Disease Vulnerability Index (IDVI), which expands the scope of analysis to other factors such as demographic and environmental indicators.
- Excludes countries with a population smaller than 1 million
- Excludes high income countries
- Excludes high income and upper middle income countries
Sources
Global Health Security Index (2019)
GSMA Mobile Connectivity Index (2018)
International Labour Organization (2018)
International Labour Organization (2018)
International Labour Organization (2020)
International Telecommunications Union (2019)
World Health Organization (2015)
Y Analytics aggregates credible findings from leading institutions and researchers. Our goal is to shine a light on the facts made available by content experts and present the implications of these facts. If you have recommendations for additional reputable data sources, insights to help us refine our analysis, or suggested research topics, please contact us at info@yanalytics.org.